- Afghanistan
- Africa
- Budget Management
- Defense
- Economy
- Education
- Energy
- Environment
- Global Diplomacy
- Health Care
- Homeland Security
- Immigration
- International Trade
- Iraq
- Judicial Nominations
- Middle East
- National Security
- Veterans
|
Home >
News & Policies >
July 2001
|
Improving Medicare Benefits
"Medicare’s current benefits were modeled on a good private insurance plan – from 36 years ago, in 1965. Back then, the primary concern was hospital costs. Today, many seniors are treated at home, or in a doctor’s office, with drugs and new medical technologies. Back then, in 1965, the focus was acute care. Today, there is a greater emphasis on preventive care. Medicare is an enduring commitment of our country. It must be modernized for our times."
-- President George W. Bush
When Medicare was created in 1965, the benefit package was based on the most popular Blue Cross/Blue Shield insurance policy offered at the time. Since then, medicine has changed profoundly, and the health insurance options available to most Americans have changed along with it. Yet Medicare’s benefit package has in many ways remained rooted in the 1960’s. Medicare’s coverage of many treatments is often delayed by years or even decades, as in the case of prescription drugs. Even when treatments are covered, Medicare’s patchwork benefits have serious gaps, as too many seniors discover when they experience serious illnesses. These problems are illustrated not only by prescription drugs, but also by other types of care such as preventive medicine and treatments that provide alternatives to major surgery.
Prescription Drugs
One of the most glaring omissions in Medicare’s benefits is the lack of prescription drug coverage. Prescription drugs are an increasingly important part of effective health care. They are used to relieve pain, enhance the lives of millions of Americans, and reduce health care costs by avoiding more costly treatments, hospitalizations, and complications. For example:
- Serious complications such as gastrointestinal bleeding and abdominal surgery for ulcers are becoming much less frequent because of drug treatment with a combination of antibiotics and proton pump inhibitor drugs. Innovative drugs can eliminate the cause of the vast majority of ulcers for less than $500, preventing prolonged hospitalizations costing upwards of $28,000.
- A year’s worth of treatment with blood thinning drugs known as anticoagulants, which reduce strokes in patients with a common heart problem called atrial fibrillation, costs less than $1,000 per year. In contrast, lifetime medical costs related to a serious stroke exceed $100,000.
- Drugs called statins can reduce heart attacks in older persons at risk for them and may reduce the risk of stroke and possibly other conditions, avoiding costly hospitalizations and many complications and deaths from cardiovascular disease.
- Drugs that promote calcium absorption into bones have been shown to significantly reduce serious complications of osteoporosis in older women, including the risk of hip fractures. Hip fractures often lead to long and costly hospitalizations, nursing home admissions, and even death.
In the past decade alone, almost 400 new drugs have been developed to fight cancer, heart disease, stroke, diabetes, Parkinson’s disease, depression and arthritis. Thanks to active investment in research, still more effective prescription drugs are expected to reach seniors in the years ahead. These include treatments for a host of conditions ranging from breast and prostate cancer and to Alzheimer’s disease.
Over 98 percentThe vast majority of employer-sponsored health plans have long recognized the value of medicines in keeping people healthy and therefore provide drug coverage as part of their benefit package. Private Even though private plans began covering prescription drugs by the mid-1960s., Medicare’s benefit package has yet to havestill has not been updated to include drugs, even though drugs are an increasingly important part of seniors’ medical care. Nine out of ten Medicare beneficiaries will use at least one prescription drug thisthis year, and the proportion of seniors who incur very high drug expenses is growing. As a result of the use of these valuable but costly new treatments, prescription drug spending is expected to continue to grow at the rate of 12.6 percent a year for in the coming decade.
Without coverage from Medicare, most seniors have coverage from other sources (see Chart 1).
CHART 1
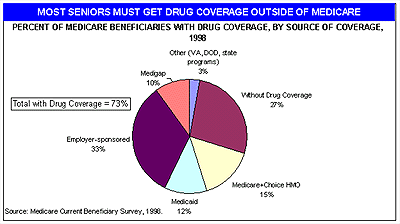
Overall, about 27 percent of Medicare beneficiaries do not have prescription drug insurance and must pay for prescription drugs entirely out of their own pockets or go without needed drugs. Worse, this financial burden falls heaviest on those least able to afford it, and the impact on their health care may be significant. A recent study found that Medicare beneficiaries without prescription drug coverage used 8 fewer prescriptions a year than the seniors with coverage. The differences for low-income seniors were even greater – those—those without drug coverage used 14 fewer prescriptions than low-income seniors with coverage.
Quality private-sector prescription drug benefits not only protect seniors from the risk of high prescription drug expenses; t, they also help make all prescription drugs more affordable through innovative tools to help beneficiaries reduce their drug costs. Private insurance plans usually work with "pharmacy benefit managers" to provide these tools, which include:
- Competitive buying power to negotiate volume discounts: The benefit managers for lLarge private insurance plans and the benefit managers each represent many people who are likely to purchase drugs through their benefit. Thus, they can negotiate effectively to get the best drug pricesprices on drug purchases.
- Assistance for seniors in choosingBetter information for people and their doctors on prescription drugs: By working with pharmacies and physicians to provide individualized providing information on more -effective and lower-cost drug options, benefit managers they can improve the quality of seniors’ prescription drug use. Their computerized support systems can also help avoid adverse drug interactions, which are far more common in seniors than in any other part of the population.
According to a recent analysis by the Congressional Budget Office, these private-sector tools could save seniors significantly more than the savings that would be achieved through a government-run prescription drug plan. In addition, giving seniors a choice of options helps ensure that they will be able to use receive the drugs and pharmacies that they prefer.
Because a government-run plan will not be able to control drug costs as effectively, the higher prices would be likely to lead to permanent government price controls. In other industries where permanent price controls have been implemented, the result has been less supply and less innovation. President Bush believes that employing private sector tools can increase access to prescription drugs and encourage the development increase investment and discovery of even more valuable drugs in the future.
Preventive Care
Medicare’s coverage of proven treatments for preventing illnesses and saving lives has also lagged. Coverage often comes long after preventive treatments are widely covered in private insurance plans. For example:
- Mammograms: Mammograms were first shown to save lives in the early 1980s by permitting breast cancer to be treated at a curable stage. Medicare did not cover annual mammograms until 1998.
- Prostate cancer screening: Tests were widely available in private health plans by the late 1980s. Medicare coverage did not begin until 2000.
- Prostate cancer screening: Tests were widely available in private health plans by the late 1980s. Medicare coverage did not begin until 2000.
- Flu vaccines: Flu vaccinations have been known to avoid serious complications from respiratory illnesses since the 1970s. Medicare did not begin coverage until 1993.
Even though these and other treatments such as colonoscopies and preventive care for diabetes have finally been covered, Medicare usually imposes significant copayments of 20 percent on the cost of preventive care. In addition, Medicare’s coverage of many preventive services does not begin until beneficiaries have exceeded Medicare’s $100 Part B deductible. As a result, healthy Medicare beneficiaries can frequently face costs in the hundreds of dollars each year, just to keep up with recommended preventive treatments. Medicare’s coverage of preventive care stands in contrast to the best private health insurance plans. Private plans have moved to a stronger emphasis on disease prevention by reducing beneficiary payments for preventive care, or even by making very cost-effective preventive services free.
Serious Illnesses
The development of new technologies and new treatments for the most serious illnesses, such as intensive life support for patients with major heart attacks, makes it possible for more people seniors to survive potentially fatal illnesses. Unfortunately, Medicare beneficiaries who are sickest often pay the highest share of their health care costs – exactly the opposite of the way that logical insurance plans work. For example:
- Medicare’s copayments for outpatient procedures related to serious illness, such as arthroscopic procedures on joints and complex chemotherapy treatments for cancer, may exceed 40 or 50 percent. Beneficiaries who have to undergo extensive or multiple outpatient procedures – such as cancer patients undergoing a course of treatment or diabetes patients who require multiple treatments for complications – may have thousands of dollars in Medicare cost-sharing obligations.
- People who require longer stays in skilled nursing facilities – for example, patients who have severe strokes or frail patients recovering from a hip fracture – face copayments of almost $100 per day.
- Individuals who need hospital care currently face a payment of almost $800 for each hospital spell. This payment is far higher than in virtually all private plans, which have a single deductible and a simpler copayment system. According to analyses by the Centers for Medicare and Medicaid Services, hospitalizations are common for Medicare beneficiaries. Even though less than one in five beneficiaries has a hospital stay in any one year, about half of beneficiaries require hospital care over a 5-year period, and about one in three beneficiaries have two or more hospitalizations. In addition, Medicare beneficiaries with who require extremely long acute hospital stays are exposed to daily copayments that run into the hundreds of dollars, and Medicare coverage can eventually run out altogether. Medicare’s coverage of hospital stays is far less generous than the standard Blue Cross/Blue Shield plan offered to all Federal employees (see Chart 2).
CHART 2
|
MEDICARE DOES NOT PROTECT AGAINST SERIOUS ILLNESS |
||||
| Beneficiary Pays: | ||||
|
Days 1-60 |
Days 61-90 |
Days 91-150 |
Over 150 days |
|
|
Medicare |
$792 payment per hospital spell |
$198 per day |
$396 per day |
All costs |
| Standard Blue Cross/ Blue Shield Plan for Federal Employees |
$100 payment per hospital admission |
$0 per day |
$0 per day |
$0 per day |
These substantial cost-sharing requirements add up. Beneficiaries who incur costs of $25,000 or more are on average responsible for over $5,100 in cost-sharing due to Medicare’s deductibles, copayments, and coverage limits. With modern technology, such costs are not that uncommon: t The cost for treating a patient with heart disease who needs an implantable defibrillator exceeds $35,000. To protect beneficiaries when they need help the most, private insurance plans generally include "stop-loss" limits. Stop-loss limits provide guaranteed protection against very high medical expenses. Despite its important coverage gaps, Medicare has no stop-loss protection.
Supplemental Insurance
Because of the limitations in Medicare’s benefit package outlined above, it is not surprising that six out of seven seniors in the traditional plan get supplemental or "wrap around" insurance to help fill Medicare’s gaps. Some seniors get supplemental insurance from Medicaid, if their incomes are low enough. Others have employer-subsidized supplemental coverage as a retirement benefit. But a growing number of seniorsMedicare beneficiaries do not have any of these options. They mustface a choice: either purchase individual supplemental insurance, called such as Medigap, risk burdening family and friends in the event of serious illness, or forego care altogether. Supplemental Not surprisingly, six out of seven beneficiaries in Medicare’s traditional plan obtain supplemental insurance. insurance is an essential part of the Medicare programBut as Medicare’s gaps have grown, so have supplemental insurance premiums. Supplemental insurance premiums now account for over one-fifth ofa larger share of beneficiaries’ total payments for all types of medical careout-of-pocket spending than any other type of medical expense and exceed prescription drug and dental expenses. combined According to AARP, supplemental insurance premiums were projected to cost even more on average in 1999 than did premiums for Medicare insurance and more than spending on prescription drugs and long-term care combined (see Chart 3).
CHART 3
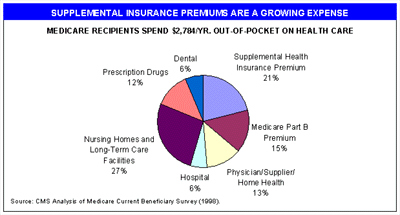
Individual Medigap coverage is the only option for better coverage for a growing number of beneficiaries. But asAs seniors receive more costly treatments with with high cost sharing copayments, Medigap premiums risehave to go up. While the costs of the policies that provide some drug coverage have grown very rapidly, premiums for Medigap plans without drugs have also increased over the past 3 years – by 25 to 45 percent. By comparison, the Medicare Part B premium is both much lower than Medigap premiums and has increased by much less over the past 3 years – only 4 percent.
Because of the rising cost of current Medigap options, some seniors may prefer more affordable alternatives. Insurance experts who have analyzed the standard Medigap options have identified uncovered several components of the cost problems that increase the price of supplemental insurance:
- Medigap coverage of the Medicare Part B deductible is "dollar trading," in the sense that beneficiaries pay for the amount of the deductible whether or not they get Medigap. Either they pay the first $100 of Medicare benefits, or they pay a premium for Medigap that is more than $100 higher than the premium for Medigap that does not cover the deductible. (The amount is over $100 because of loading costs for the Medigap companies.)
- "First-dollar" Medigap coverage also leads to higher Medicare and Medigap costs. Academic researchers and the nonpartisan Office of the Actuary estimate that service use is 23 percent higher for beneficiaries with Medigap than for beneficiaries without supplemental insurance. Medicare pays most of these costs, but they also lead to higher Medicare and Medigap premiums. According to the General Accounting Office, even modest changes in first-dollar coverage would lead to significantly lower Medicare costs, and in turn lower Medigap costs. The substantial budgetary costs of first-dollar coverage also contributes to the delays in covering new technologies in Medicare.
- The cost of covering Medicare’s high payment for each hospitalization, and of providing the protection against high out-of-pocket expenses that Medicare does not provide, both contribute to rising Medigap premiums. Reducing the Part A hospital deductible and providing protection against very high expenses would result in more affordable Medigap options, because supplemental insurance would no longer have to cover these costs.
Almost all private insurance plans avoid first-dollar coverage and instead use reasonable copayments. Private plan enrollees have some limited out-of-pocket costs to help encourage appropriate use of services, and the enrollees benefit from much lower insurance premiums. Private insurance plans also take other effective steps to make sure that small copayments do not discourage appropriate care. These include, such as providing extra incentives for patients and physicians to use preventive care that avoids complications, and implementing programs to encourage appropriate management of chronic illnesses.
The President’s Framework for Improving Medicare Benefits
The President will work to improve Medicare benefits for all seniors based on the following principles:
Principle #1: All seniors should have the option of a subsidized prescription drug benefit as part of modernized Medicare.
Medicare’s subsidized drug benefit should protect seniors against high drug expenses and should give seniors with limited means the additional assistance they need. The drug benefit should give all seniors the opportunity to choose among plans that use some or all of the tools widely used in private drug plans to lower drug costs and improve quality of care. The drug benefit should support and encourage the continuation of the effective prescription drug coverage now available to many seniors through retiree plans and private health insurance plans. The new drug benefit should also be available through Medigap plans and as a stand-alone drug plan for seniors who prefer these choices. When Medicare implements the drug benefit, states should not face maintenance of effort requirements for their own drug programs outside of Medicaid.
Principle #2: Modernized Medicare should provide better benefits coverage for preventive care and serious illnesses.
Medicare’s existing coverage should be improved so that its benefits provide better protection when serious illnesses occur and provide better coverage to help prevent serious illnesses. These changes should not reduce the overall value of Medicare’s existing benefits.
- Medicare’s preventive benefits should have zero copayments and should be excluded from the deductible.
- Medicare’s traditional plan should have a single indexed deductible for Parts A and B to provide better protection from high expenses for all types of health care.
- Medicare should provide better coverage for serious illnesses, through lower copayments for hospitalizations, better coverage for very long acute hospital stays, simplified cost sharing for skilled nursing facility stays, and true stop-loss protection against very high expenses for Medicare-covered services.
- Medicare’s traditional plan should have a single indexed deductible for Parts A and B to provide better protection from high expenses for all types of health care.
These changes should not reduce the overall value of Medicare’s existing benefits.
New Medigap options, which must must be created for beneficiaries who choose the improved traditional plan with the new drug benefit, should give beneficiaries lower-cost options for reducing their out-of-pocket payments. These Medigap plans should begin by giving beneficiaries better protection against high expenses, and then should reduce Medicare’s deductible and copayments.
Principle #3: Today’s beneficiaries and those approaching retirement should have the option of keeping the traditional plan with no changes.
Many beneficiaries people in Medicare today, and others those who are approaching retirement, have good supplemental coverage for prescription drugs and other medical expenses in Medicare. If they wish to continue continue in this coverage in the traditional Medicare plan with no changes in their premium, benefits, or supplemental coverage, they should be able to do so. To make sure that they choose the option that is best for them, beneficiaries who opt for modernized Medicare should be allowed to switch back to the original plan for a yearBeneficiaries who opt for the improved Medicare benefits should be allowed for a year to switch back to the original plan.
Providing Reliable Health Insurance Options for Seniors
"Medicare beneficiaries should have the same kind of reliable coverage options available to all Federal employees throughout the country – a system that has been proven to provide one of the highest levels of satisfaction of any health care program in the country."
-- President George W. Bush
Medicare has lagged behind in providing reliable health insurance benefit options for beneficiaries that best meet their beneficiaries’ own circumstances and preferences. The Federal government, many state governments, and most large private employers help their employees get the care that is best suited to their needs by offering them several health care plans, along with unbiased and useful information to help them choose the best one. Medicare has failed to provide America’s seniors with the same kind of reliable health care options that every Federal employee has received for decades. For many beneficiaries, particularly those in rural areas, Medicare offers only one health insurance plan – it is strictly one-size-fits-all. Previous legislation to address this problem, including the establishment of the Medicare+Choice program, has not had the intended effect of providing more reliable health insurance options for Medicare beneficiaries.
The effects of Medicare’s current shortcomings can be seen very clearly in our Nation’s capital. Federal employees and Members of Congress living in Washington have twelve different health plans to choose from, including a variety of fee-for-service plans, and health maintenance organizations (HMOs). But their neighbors with Medicare coverage have only two choices – the traditional fee-for-service plan and a single HMO (see Chart 4). This pattern occurs throughout the country. Park Rangers living in the most remote national forests, and postal workers in every neighborhood, have at least seven plan choices.
CHART 4
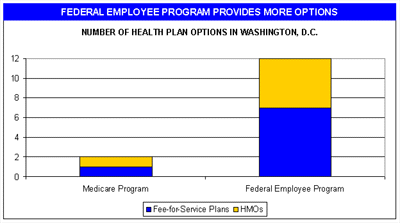
The Benefits of Better Options
Private plans will be the best will be the best option for many many seniors because:
- Private plans often have provided innovative new health benefits – including preventive care, prescription drug coverage, and dental services – without having to wait for an act of Congress. Private plans also invented state-of-the-art coordinated care for the many Medicare beneficiaries who have multiple or chronic health problems.
- Private plan options allow seniors to reduce or eliminate their co-payments and deductibles so that their out-of-pocket payments are manageable without having to purchase a supplemental insurance policy.
- Private plan options give seniors more power. If they are not happy with the service they are receiving, they can simply switch to a different plan. Competition is the best way to make bureaucracies and health plans responsive – by giving customers the freedom to choose. Medicare beneficiaries should have the same options as working Americans.
Private plan options give seniors more power. If they are not happy with the service they are receiving, they can simply switch to a different plan. Competition is the best way to make bureaucracies and health plans responsive – by giving customers the freedom to choose. Medicare beneficiaries should have the same options as working Americans.
Around one-third of seniors do not have access to any of these opportunities. And no seniors have access to new kinds of private insurance that have become popular with other Americans, such as "point of service" plans that give beneficiaries the cost savings of networks of providers along with the flexibility of coverage for services from all providers.


